PREVENTION OF CRANIOMANDIBULAR DISORDERS IN CHILDREN AND ADOLESCENTS: A CASE REPORT Sánchez ME.
Associate Professor in the Department of Prophylaxis, Pediatric Dentistry and Orthodontics, Faculty of Dentistry, Madrid Complutense University, Spain, maresanc@odon.ucm.es
Postal Address:
Mª Esperanza Sánchez Sánchez
Departamento de Profilaxis, Odontopediatría y Ortodoncia
Facultad de Odontología
Universidad Complutense de Madrid
Avda. Complutense.
Madrid 28040
Spain
Phone ns: 00 34 91 3941959
00 34 91 3941972
00 34 600737204
Abstract: Although Craniomandibular Disorders (CMD) mainly tends to affect adults, various studies have also detected the presence of signs and symptoms of CMD in children and adolescents. Its varied semiology and multi-factor etiology mean that it is often not diagnosed early enough to prevent future problems. The purpose of this paper is to present a case of early CMD in a 12-year-old girl. She was attended the Odontology Department at the Madrid Complutense University (UCM) for a check-up. Dentine wear facets, along with other indications of possible CMD, were observed when taking the case history and during the clinical examination. A more exhaustive study led to a diagnosis of compensated CMD as the patient did not present symptoms. We believe that only an early diagnosis of the semiology of CMD can allow an appropriate clinical prevention and management of the risk factors that may trigger CMD in the future.
Keywords: Craniomandibular Disorder, Child, Preventive Dentistry.
INTRODUCTION
Craniomandibular Disorders (CMD) covers a range of pathologies that arise as a result of changes to the relationship between the various components of the Stomatognathic System (SS) (1). It tends to occur more frequently in adults than in children. Despite this, the characteristic signs and symptoms of CMD are often found in the infant population (2,3) and tend to increase with age in adolescents and young adults (1,2,4,5,6).
A multi-factor etiology in which no single factor predominates is widely accepted for CMD (2,5,6,7,8).Likewise, the semiology may include the involvement of some or all of the components of the SS, especially the dentition, muscles and Temporomandibular Joints (TMJs), each of which presents a specific structural tolerance. If this tolerance is exceeded as a result of a local or systemic alteration, the weakest component will show the first sign or symptom of disease (9).
CASE REPORT
A 12-year-old girl visited the Odontology Department at the Madrid Complutense University (UCM) for a check-up. A case history and clinical examination showed permanent dentition, mild class II bilateral canine, general enamel mineralisation defects (Figure 1) and possible wear facets in some teeth that were more marked in permanent maxillary right lateral (Figure 2). She presented no signs of muscle hypertrophy, although she experienced pain upon palpation of the masticatory muscles. Intra- and extra-auricular static and dynamic palpation of both TMJs was painful. A periapical X-ray of permanent maxillary right lateral showed a greater condensation of the bony ridge between permanent maxillary right lateral and permanent maxillary right canine and a broadening of the periodontal ligament in permanent maxillary right lateral, but no fracture lines or infection foci.
An occlusal analysis was performed using a semi-adjustable articulator (Dentatus) and the Lauritzen Gnathological System in light of suspected CMD (Figure 3). The results of this study showed that the maximum intercuspation (MI) did not coincide with the centric relation (CR); there was a lack of canine guidance on the right side which was being provided by permanent maxillary right lateral and permanent mandibular right lateral, thus coinciding with the wear facets (Figure 4). The parents were asked to complete a questionnaire designed by us containing questions regarding the various CMD risk factors identified in the literature consulted. This showed that the patient presented headaches and parafunctional habits, her teeth were sensitive to cold stimuli and that she was a nervous child. These findings allowed us to confirm the presence of a compensated CMD, in other words the examination detected signs of dysfunction but the patient did not yet exhibit any symptoms. To prevent decompensation of the CMD, the patient was recommended to follow a series of preventive measures based on the findings reported in the literature consulted. These measures included eliminating parafunctional habits (nail-biting, chewing pens, chewing gum), avoiding stress and attempting not to sleep on her right-hand side to avoid using the tooth presenting the most marked wear facet (12). She was also advised to undergo orthodontic treatment to achieve correct canine guidance and a stable occlusion around the centric relation. DISCUSSION
The patient presented all the risk factors proposed to cause CMD by the majority of authors.
Although the incidence of this syndrome is higher in females (2,4,6,10) , the reason why some women are more susceptible to musculoskeletal pain, especially during the early stages of puberty, remains unknown (11).
The parafunctional habits presented by the patient (teeth-clenching, nail-biting and chewing pens and gum) are considered to be etiological factors for CMD, especially amongst the young (2,3,5,12,13,14) .
Our patient presented occlusal alterations, including the absence of a bilateral canine guidance, multiple non-working-side contacts, diastemas in various locations and an absence of concordance between the centric relation and the maximum intercuspation. Various studies have suggested occlusal anomalies to be classical etiological factors in the development of CMD(15) . CONCLUSSIONS
- This paper describes an adolescent with signs of CMD that could be overlooked or mistaken for another condition. Therefore, a detailed case history and clinical examination should be performed in children and young people in order to ensure an early diagnosis of CMD.
- The weakest component of our patient's SS was the dentition (generalised demineralisation). As a result, the first sign of CMD was wear facets.
- Orthodontic treatment to achieve an appropriate condyle fossa position is particularly suitable for preventing the development or decompensation of a CMD in the event of occlusal alterations. Parafunctional habits in children should be eliminated and psychological factors that may lead to CMD in pubescent children should be controlled, as well. 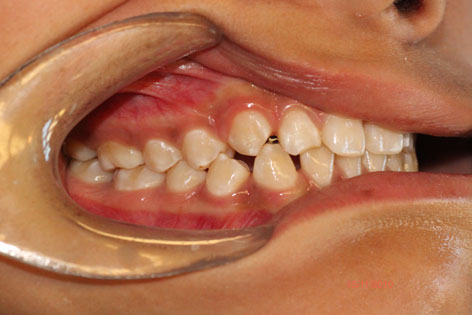 Figure 1 Occluded dental arches showing the generalised enamel defects. 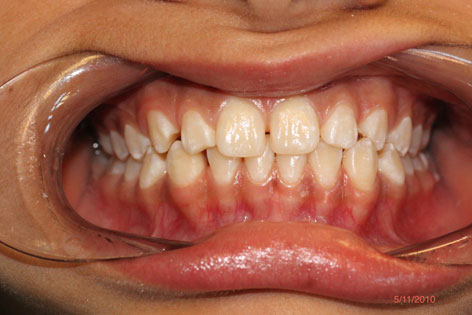 Figure 2 Wear facet in permanent maxillary right lateral due to absence of right canine guide 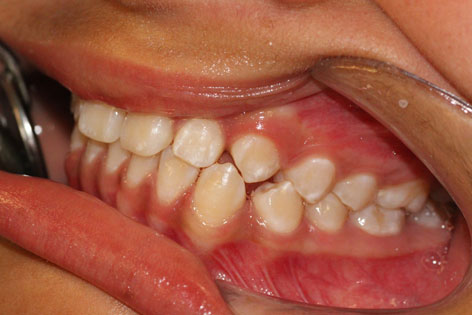 Figure 3 Casts mounted in the articulator using the Lauritzen Gnathological System. 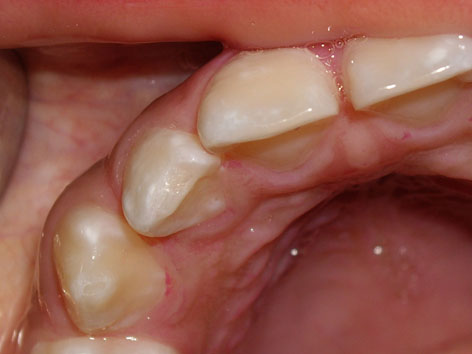 Figure 4 Occlusal analysis showing that, on the right side, guidance is provided by permanent maxillary right lateral and permanent mandibular right lateral . 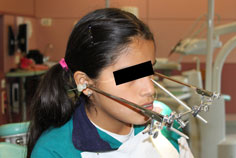  REFERENCES
1. Thilander B, Rubio G, Pena L, de Mayorga C. Prevalence of temporomandibular dysfunction and its association with malocclusion in children and adolescents: an epidemiologic study related to specified stages of dental development. Angle Orthodontist 2002; 72 (2): 146-54.
2. Pereira LJ, Pereira-Cenci T, Del Bel Cury AA, Pereira SM, Pereira AC, Ambrosano GM, Gaviao MB "Risk Indicators of Temporomandibular Disorder Incidences in Early Adolescence". Pediatr Dent 2010; 32(4):324-8.
3. Seraj B, Ahmadi R, Mirkarimi M, Ghadimi S, Beheshti M Temporomandibular Disorders and Parafunctional Habits in Children and Adolescence: A Review. J Dent 2009;6(1):37-45.
4. Nilsson IM, Drangsholt M, List T "Impact of Temporomandibular Disorder Pain in Adolescents: Differences by Age and Gender". J Orofac Pain 2009; 23 (2): 115-22.
5. Michelotti A, Coffi I, Festa P, Scala G, Farella M. Oral parafunctions as risks factors for diagnostics TMD subgroups. J Oral Rehabil 2010;37:157-62.
6. Miller JR, Mancl L "Risk factors for the occurrence and prevention of temporomandibular joint and muscle disorders: Lessons from 2 recent studies". Am J Orthod Dentofacial Ortop 2008; 134(4):537-42.
7. Greene CS. The etiology of temporomandibular disorders: Implications for treatment. J Orofac Pain 2001;15(2):93-105.
8. Leresche L, Mancl LA, Drangsholt MT, Huang G, Von Korff M. Predictors of onset of facial pain and temporomandibular disorders in early adolescence. Pain 2007;129:269-78.
9. Pozo JJ, Pérez MD, Casado JR. Disfunción del aparato estomatognático. Semiología neuromuscular. Rev Eur Odonto-Estomatología 2004; 16 (3): 123-34.
10. Winocur E, Littnerusb D, Adamsusb I, Gavish A. Oral habits and their association with signs and symptoms of temporomandibular disorders in adolescents: a gender comparison. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2006;102:482-7
11. Ferreira CL, da Silva MA, de Felício CM "Orofacial Myofunctional Disorder In Subjects with Temporomandibular Disorder". Cranio 2009;27(4):268-74.
12. Emodi-Perlman A, Eli I, Friedman Rubin P, Goldsmith C, Reiter S, Winocur E. Bruxism, oral parafunctions, anamnestic and clinical findings of temporomandibular disorders in children. J Oral Rehabil 2012; 39; 126-35.
13. Cortese SG, Biondi AM. Relationship between dysfunctions and parafunctional oral habits, and temporomandibular disorders in children and teenagers. Arch Argent Pediatr 2009;107(2):134-38.
14. Magnusson T, Egermark I, Carlsson G. A prospective investigation over two decades on signs and symptoms of temporo-mandibular disorders and associated variables. A final summary. Acta Odontol Scand 2005;63(2):99-109.
15. American Academy of Pediatric Dentistry Clinical Affairs Committee-Temporomandibular Joint Problems in Children Subcommittee; American Academy of Pediatric Dentistry Council on Clinical Affairs. "Guideline on acquired temporomandibular disorders in infants, children and adolescents". Pediatr Dent 2011:Special Issue 33 (6): 248-53.
|





